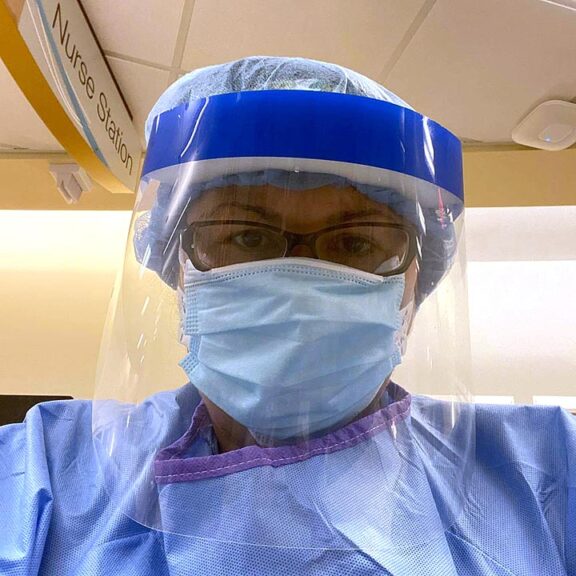
Yellow Springs resident Chasilee Crawford is an ICU, or intensive care unit, nurse at Springfield Regional Medical Center. She volunteered to work in the hospital’s designated COVID-19 specific ICU when it was formed last March, and has been caring for patients who are severely ill with the disease ever since.
Caring for COVID’s sickest patients
- Published: December 22, 2020
“I cried at work yesterday. It seems I’ve been doing that a lot lately, but yesterday was especially hard.”
Chasilee Crawford, an ICU nurse working in the COVID-19 unit at Springfield Regional Medical Center, recently turned to Facebook with a widely shared post describing her sadness, weariness and frustration in fighting the pandemic that has seen a growing surge in recent weeks:
“I had two patients, one younger than me and one only a few years older. Both fighting for their lives from the coronavirus,” the post continued. “I thought I was going to lose my young patient yesterday after we intubated her. But between the respiratory therapist and my coworkers, we managed to prone her immediately and she survived. I spent the rest of the day stabilizing her. Before we intubated, her husband called me and begged me to come see his wife. He just wanted to hold her hand one more time. I couldn’t let him do it. The best I could offer was a FaceTime or Zoom call. I cried again. Every time the doctors would come in, they would just shake their heads, some had tears in their eyes as well. I cried again. All day long, I heard codes overhead, heard helicopters in the air, and saw people (my coworkers) running the halls. At the end of the day, I finally sat down, put my head on the desk and said a prayer for my patients, coworkers, and everyone who has been affected by this nasty virus. Please wear a mask, social distance, and stay safe! F**K COVID!”
“It was just one of those hard days,” Crawford said with a sigh in retrospect, a rueful smile revealing some self-consciousness about the attention her Facebook post has received. In an interview conducted by Zoom last weekend, the Yellow Springs resident said there have been a lot of hard days since the COVID unit was formed last March.
And while the number of patients and extreme cases went down over the summer, they have continued to rise in recent months to the extent that her hospital is anticipating opening an additional, third unit, dedicated to COVID treatment, she said.
She said the hospital administration established the first unit in late winter, with a plan to open a second unit if necessary. The “first wave” of patients hit in March, but the second unit wasn’t needed until this fall.
“We always knew that it was going to get much worse,” Crawford said. “So we were prepared,” at least administratively in terms of beds and supplies. Mental preparation is harder, she said.
“It is taking a toll on us, physically, mentally,” she said.
A COVID unit at her hospital has 30 beds total, with the COVID ICU, for those needing intensive care, supporting eight dedicated beds, Crawford said.
COVID patients are classified ICU if they need to be on a mechanical ventilator to help them breathe. The procedure involves inserting a tube (intubation) into the patient’s trachea (the large airway between the mouth and the lungs) and requires that the patient be sedated and then often kept in a semi-conscious state because of the invasive discomfort of the apparatus.
“These are sick, sick, sick people,” Crawford said.
As of last weekend, the hospital had 14 ventilated patients, nearly twice as many as the designated COVID ICU beds, she said.
“We did not have enough ICU nurses for those patients; the step-down nurses had to take on their care,” Crawford said, adding that those nurses are qualified, just not typically assigned to intensive care, where nurses generally have oversight for two — sometimes one, sometimes three — patients. “I wouldn’t say we are understaffed.”
At the same time, “nurses are taxed,” she said. “Our patients are so fragile. One minute they can be fine, and the next minute they need a ventilator.”
She said the patient whose intubation she described in her Facebook post is 47 years old.
“I walked in, I knew this patient was struggling. I knew the best thing was being put on a ventilator.” But the procedure can also take a physical toll.
Crawford said it isn’t unusual for a patient’s body to “relax” too much after intubation.
“You’re struggling to breathe for so long — it can get harder and harder and harder,” she said. “The patient, she had no reserves.” Once the ventilator was doing its job, “her lungs relaxed, and they didn’t want to work anymore.”
“We just had to fight for her.”
“That’s what we do,” Crawford added. “We fight for our patients every day. It’s a battle. It really is a battle.”
Crawford, like many other nurses in her unit, volunteered for her current assignment, she said.
“We know these people need care,” she said simply.
Prior to the pandemic, Crawford had been part of the hospital’s general Intensive Care Unit for three years, coming to Springfield from the ICU at the now closed Good Samaritan Hospital in Dayton. She worked in the in-patient trauma center at Miami Valley Hospital before that, taking the job after moving to the area with her family from her birth state of Oklahoma.
She said she wanted to go into the medical professions as a child, initially intending to become a doctor. Her first job while still in school was as a nurse’s assistant, and it was then she decided that nursing offered more of what she wanted in her career.
“I saw the nurses around me and what they were doing and how they cared for their patients,” she recalled. “I wanted to be hands on. I wanted to provide patients with the medical aspects, but be that person that’s hands on, not just give a diagnosis and then leave.”
“Not to undermine what the doctors do,” she added. Nursing has a different emphasis, though, putting in hours of direct care, and serving as “the eyes and the ears for the doctors.”
Certified as a licensed professional nurse, or LPN, in 1993, Crawford became a registered nurse, or RN, in 2013. In addition to her current job, she is also completing clinical requirements — assigned to Rocking Horse Center in Springfield — in becoming a nurse practitioner, who can diagnose and prescribe medication.
As a nurse, Crawford said she attends not only to the needs of her patients, but also their families, especially in the COVID unit, where patients are isolated from visitors. In talking about her responsibilities, she speaks not only of “my patients,” but also “my families.”
“COVID is so hard,” she said. “Family members can’t be with their patients.”
The unit nurses try to keep families informed about what’s happening with their hospitalized loved one, facilitate phone calls or video chats if possible, and help them process their fears and sometimes grief.
“Is my loved one going to make it?” is a common question. Crawford can say in all honesty that the doctors and nurses will do everything they can to see they do, but she can make no promises.
As an experienced ICU nurse, who also has done hospice care in the past, Crawford is familiar with death, and has learned to focus on the act of giving patients the best care she can in the moment.
“It’s satisfying to go home and know that you did everything in your power today to make sure that person is on the spectrum of life where they need to be,” she said.
The days are admittedly long, with a typical shift lasting 12 hours. That doesn’t include the time needed to suit up in appropriate protective gear beforehand and to clean up afterward. Crawford clocks in at 7 a.m wearing a surgical gown, scrubs, “a hat to cover my hair,” goggles, an N95-style face mask and a paper mask over it. She, like her colleagues, also puts all of her ID badges, “all of our things that could possibly be exposed,” in baggies. At the end of the shift, staff put their belongings in what they call the “easy bake oven,” an ultraviolet oven that kills viruses. They clean off their shoes with bleach wipes; wash themselves, with many taking a shower before leaving; and put on clean clothes.
“Sometimes I don’t get home until 9 p.m.,” Crawford said.
With a daughter in high school, Crawford said she’s been fortunate that her mother came in from Oklahoma to help out at home. But she also worries about passing the virus on to her family, especially her elderly mother. She’s been strict about following guidelines from the Centers for Disease Control concerning mask wearing and social distancing in public.
She said the hospital has been successful in controlling internal spread of the disease, with a handful of employees testing positive over the past nine months, and none contracting a serious case.
“I’m grateful for that,” she said.
She said that while some of her colleagues become upset by people who deny the severity of the pandemic and refuse to wear a mask or follow other pre-emptive measures, she doesn’t spend energy on something she can’t control.
“I do what I can do to protect myself, to protect my family, protect my loved ones, and I try to stay away from people who don’t,” she said. “I’m only doing what I can do.”
Crawford said she maintains her emotional and mental equilibrium through the support of her family and a close circle of friends, who also practice social distancing, and through plants.
“I love plants,” she said with a laugh. “I have them all over my house. Plants are life.”
She also leans on her colleagues.
“We’re such a strong team. I can’t say enough how much we rely on each other,” she said wiping away tears. “We could not do this without each other.”
“We’re nurses, we’re tired, but we continue to do this, and not because it’s our job. We love doing this. I’ve been working since March. I haven’t seen any extra benefits from the government. I don’t get hazard pay. This is basically our calling.”
One Response to “Caring for COVID’s sickest patients”
The Yellow Springs News encourages respectful discussion of this article.
You must login to post a comment.
Don't have a login? Register for a free YSNews.com account.

















Usually a thankless job, but nothing like a pandemic to shine the coal to diamond. I was married to a nurse who tried to kill me in an domestic violence situation, so I’ve never really favored them as ‘heroes’ ….. until this covid crisis. “Thanks” to ya’ll for your service. Happier Holidays ahead for all!