
Dr. Stuart "Skip" Leeds (submitted)
‘We have to trust the math’: An interview with Dr. Skip Leeds
- Published: June 6, 2020
Interviews in this series
- Jun 13, 2020 —
Yellow Springs’ own ‘Cassandra’: An interview with Dr. Allen Hunt - May 18, 2020 —
Reopening restaurants: An interview with Dan Young - Apr 26, 2020 —
COVID-19 in Greene County: Interview with an epidemiologist
Two weeks ago, Yellow Springs News editor Megan Bachman spoke with local physician Dr. Stuart “Skip” Leeds by phone to get his take on COVID-19 in the state of Ohio and Yellow Springs. He addresses masks, Ohio’s reopening plan, early pandemic projections, the possibility of a second wave and local responses to the threat.
Dr. Leeds is an Assistant Professor of Family Medicine at Wright State University School of Medicine and a member of the Wright State Physicians COVID-19 Task Force. He has been a family physician since 1998, and currently lives in Yellow Springs.
The interview was edited for length.
Yellow Springs News: You wrote a strongly worded letter to Gov. DeWine criticizing his about face on mandatory masks. Can you say more about that?
Dr. Leeds: Nothing about what I said there has changed. [DeWine] has adopted a soft libertarian approach, trusting that people will do the right thing if you ask them. You need only to spend three minutes at a Kroger to know that is not true.
Yellow Springs News: And what about the reopening? Do you think it’s happening too quickly?
Dr. Leeds: It doesn’t have a scientific basis. The math says, stop, don’t do this. It seems like the working hypothesis is that the virus is like a home invader, knocking, scratching at your door. Then when it feels like no one is home, it stalks off and you can come out. That is the model, and it has to do with our faulty human threat analysis. We’ve done so well and we’ve lowered the fatality rate. We think we have to wait it out until you’ve drained the virus reservoir, wait until the cases drop to zero, then three days later you can come out. But that’s impossible. That’s never going to happen. Human beings are teeming reservoirs of this virus. You only need one sick person and you start the whole exponential cascade over again. To further complicate matters, this virus has the annoying property of asymptomatic shedding — making you contagious even before you know you’re sick.
So there is, at best, a “wishful thinking model.” Though some appear to be working from a more cynical “social Darwinist” sort of model, which really boils down to: let old people die. The mean age [for fatalities] in Ohio is 80. That’s the center of the bell curve for the vulnerable population. And as soon as we reopen we’re going to multiply deaths by two, three, four times … and our seniors will take the brunt of it. Though it will take weeks or months for us to see the effects of our policy changes.
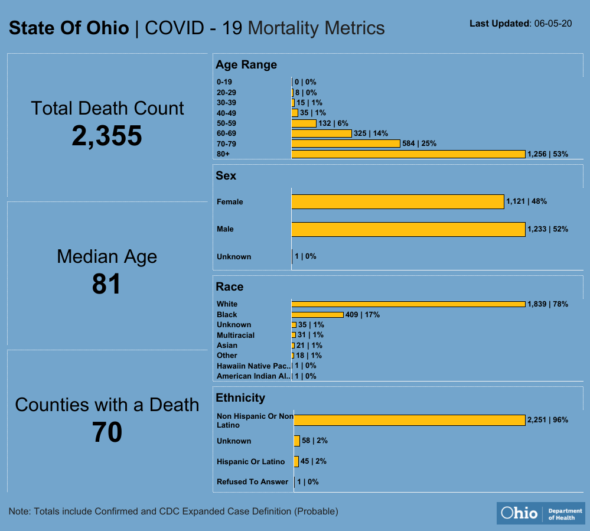
We need to understand what we’ve accomplished in the last 10 weeks. As our testing rate in Ohio is abysmal, we only have a little over 30 thousand documented cases. Let’s be generous and say that the true incidence rate is 10-fold that — so there have been 300,000 cases. In all of Ohio, 300,000 have had this infection. That’s about 3% of the state population. So all we’ve managed to do is confine the infection to that 3%. As soon as you let up on restrictions, the remaining 97% will be exposed. If, as [Professor Neil] Ferguson and other epidemiologists have said, we should assume that 40 to 70% of the population will eventually be infected…that means we’re about 1/15th of the way through this pandemic. Let’s be even more generous and say our incidence is really 10%. So instead of 1/15th, we’re really 1/5th of the way through this. Do you feel reassured?
Yellow Springs News: But didn’t we flatten the curve? And avoid 60,000 new daily cases in Ohio?
Dr. Leeds: Here’s a way to understand the flattening of the curve. When you squeeze a balloon, it’s the same amount of air, but it’s flatter. Flattening the curve redistributes the “mass” of cases over time. You make the balloon flatter, but it’s also longer. Total number of cases are conserved. There are two social-distancing strategies you can use in a pandemic: suppression and mitigation. Suppression is: you lock everyone up until it goes away. That’s what China tried to do. We continue until we eradicate the viral reservoir or come up with a vaccine or a viable treatment. Then there’s mitigation, which is flattening the curve and just stretching out the cases over time. It just buys time, and keeps us from exceeding our critical care capacity. But it’s roughly the same gross number [of cases]. There’s a reasonable argument that this is oversimplified, and that the balloon is “leaky” at the far end. That is, that total cases really are being reduced, because of factors like herd immunity — so when you get between 60 and 90% [of the population infected], the virus is gone. Sweden is trying this. Same population roughly as Ohio. But they have nationalized healthcare in Sweden. Sweden has a far greater sense of community and collective responsibility than the US. Let’s really do Sweden if we’re going to do Sweden. And I feel compelled to point out that, for all that, the Swedish experiment appears to be failing. Their fatality rate is unacceptably high, with an immunity rate around 8%, last I looked.
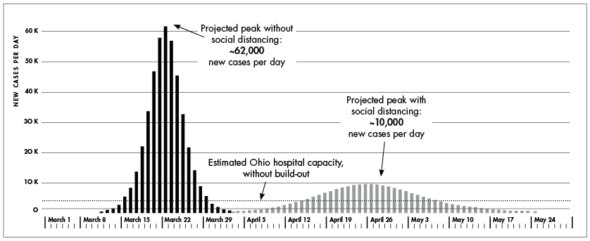
Ohio Department of Health projections on March 28. Confirmed new cases reached a peak of 1,380 on April 19.
Yellow Springs News:: Can you talk more about the issue of masks. Should Yellow Springs pass an ordinance to make them mandatory?
Dr. Leeds: Yes, without question. But if we do, we’re probably going to buy ourselves a lawsuit. It’s really clear at this point that masks work. The data is there. And risk-benefit-wise, the risk is extremely low. If you could get people to do the right thing and wear them voluntarily, that would be great. But American culture, in its current love affair with toxic autonomy, doesn’t seem to support that very well.
In specific locations, especially at the local level, if you can — make masks mandatory. On the libertarian end of things, if you have a store you can make them mandatory. On the more intrusive end, you have to wear a mask while you’re in the city limits or you could be arrested. I would go with as draconian a level as possible. As far as my medical ethics, I’m a risk-benefit analysis person. The risk is low. It’s not hard to wear a mask, but no one dies from having to wear a mask.
Yellow Springs News:: But aren’t there health conditions that exempt people from being able to wear masks?
Dr. Leeds: There are almost none. A patient recently came to me and said, “I have asthma and I want you to write me a letter to excuse me from wearing a mask at work.” And I replied that if you have asthma symptoms to the point where you can’t wear a mask, then you need to see me because your asthma is not under control. Generally speaking, a controlled asthmatic shouldn’t have a problem with masks. Do people have a negative psychological reaction to mask-wearing? Does claustrophobia cause stress, and vice-versa? Yes and yes. But for the vast majority of people, there is no physiological reason for refusing to wear a mask.
Yellow Springs News: What do you think about the Village’s decision to reopen the municipal pool?
Dr. Leeds: To me, that’s an unforced error. It’s completely unnecessary. I have two mantras that apply daily to this pandemic. One is: don’t make unforced errors. It’s a risk-benefit thing, if the benefit is low and the risk is high, that’s an unforced error. The other mantra is: don’t be an early adopter. On May 15, hair salons were permitted to reopen. My own stylist texted me and said, “I’m starting to take clients again. ” I replied that I’m not going to make an appointment until, at a minimum, June 1. A two-week delay after a policy change is really a minimum. In truth, you should probably wait a month or more because the cases and fatalities come in later. This is the problem of epidemiological latency, which is a function of disease biology, reporting delays, and other factors. If there’s going to be a second wave, you won’t know the magnitude for weeks or months. So really, you should probably wait six to eight weeks after any policy to see what the consequences will be. We won’t know [the impact of opening hair salons] until maybe the end of June. Although, because of so many things changing at once, the results of this experiment could be hard to interpret.
Our human threat analysis apparatus is terrible for any kind of delayed toxicity. We underestimate risk when the consequences aren’t immediate. That’s why people smoke — they don’t light a cigarette and die three minutes later. That perceptual blindspot will not serve us well in a pandemic. Our best antidote to this is math. This is a situation where we have to trust the math. DeWine started out trusting the math. As time wore on and the pressures built from the outside, and the economy didn’t like the timetable set by the epidemiology … DeWine and his team set aside the math and went with the decision to begin reopening on May 15.
Yellow Springs News: But wasn’t the initial math, that 60,000 Ohioans a day would contract the virus if we took no action, perhaps too pessimistic?
Dr. Leeds: Epidemics are second-order phenomena. A second-order phenomenon is affected by the predictions you make and the responses you mount to the phenomenon itself. The experiment changes as soon as you see that 60,000 are going to die and start taking steps to avoid it. As for how right those Cassandra-style predictions might have been if we’d done nothing – that’s unknowable. I’m inclined to believe that the changes we made affected the accuracy of predictions by a large margin. Unfortunately, that leads some people to the exact wrong conclusions about what happened and what we’ve accomplished. I think it’s really unfair for people to savage the initial models for doing exactly what they were designed to do: change behavior in a way that, paradoxically, makes the model wrong or obsolete. Epidemiological models are not about predicting the future. They are about making best guesses to guide response and policy.
Yellow Springs News: If you look at the state data, cases and deaths are continuing to rise, hospitalizations are flat, and ICU admissions are the only indicator showing a downward trajectory. [In the last two weeks, daily cases have also flattened and deaths are declining slightly.] What do you make of those numbers?
Dr. Leeds: Ohio has done a really good job of staying under capacity. Social distancing has probably kept the virus away from really sick, vulnerable people. If people let up, as we’re doing, the cases will start to surge again — though the critical care and fatality rates, as we discussed, will lag somewhat.
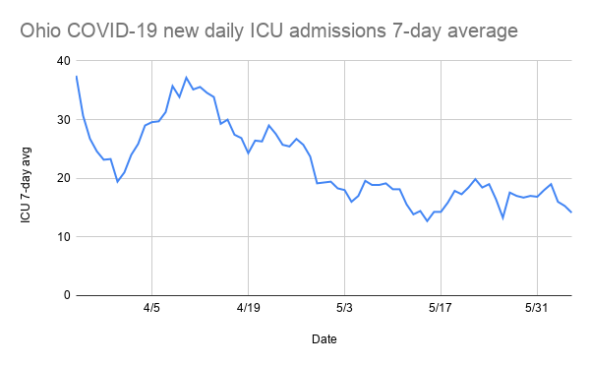
Yellow Springs News graphic with data from Ohio Department of Health
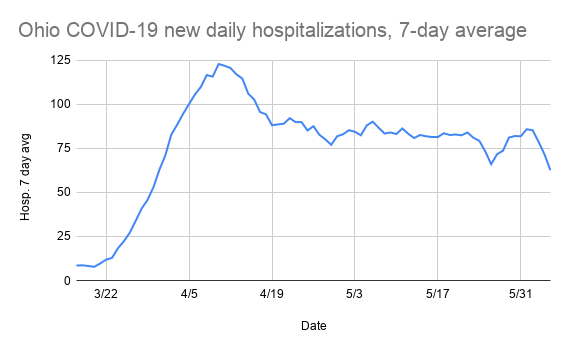
Yellow Springs News graphic with data from Ohio Department of Health
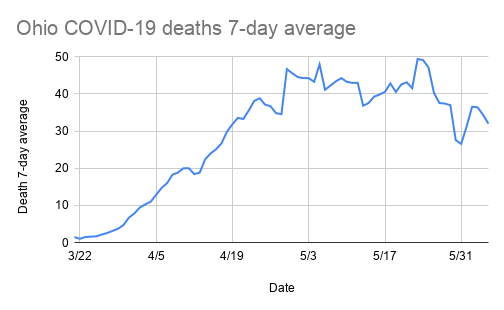
Yellow Springs News graphic with data from Ohio Department of Health
Locally, the latest policy controversy is the pool opening. Per my mantras, both an unforced error and a problem of early adoption. it’s not the water. It’s a social contact issue. I think at a pool, social distancing is basically impossible. Those things are like carnivals of chaos. You can’t keep people at a distance, it’s just the social distance and entropy factor. For me, this is a no-brainer. It’s a bad idea. There’s what you wish for in life…and then there’s math. My favorite line of pandemic poetry is: “God’s hammer is made of math.”
Yellow Springs News: But aren’t the state guidelines for reopening places like the pool based upon sound science? There is more testing, including antibody testing, there are plans for contact tracing.
Dr. Leeds: The math says we’re in trouble. The last I heard Ohio was like 46th in testing. I think we’re doing a terrible job [Update: Ohio is currently 44th in testing]. We are testing somewhere around 10,000 a day, far short of the 22,000 per day DeWine set as a target. There’s so much more I think we could and should be doing. Recently, the conservative economist Alex Tabarrok suggested in a WashPo feature that if we got rigorous about contact tracing, this pandemic be over by July 1! Economies aren’t machines. They are, as Tabarrok said, made out of confidence and hope. If people jump back into their former economic lives, and they don’t have faith that it’s safe and reasonable to do this, the economy is going to collapse anyway.
As for the antibody testing, I tell my students never order a test unless you know what you’re going to do with it. The problem with both the antibody and the viral PCR test is that we don’t exactly know what they mean. Say you have a positive antibody test now. What does it mean to have the antibodies? Are you permanently immune to coronavirus? Does it mean you can no longer be an asymptomatic carrier? We don’t know any of this with certainty. This test might, therefore, have a negative utility — i.e., it might convey a false sense of security. The PCR test, at this point, is fairly reliable. But what are you going to do with this information? It might help you decide how rigorous your quarantining should be, but the real utility is contact tracing. We’re not doing any meaningful contract tracing in Ohio, though. That’s a huge fail on DeWine’s part.
I think this speaks to the lack of coherency in our whole approach to COVID-19. If you’re not going to put people in a suppression program, or at least high-level mitigation … then you better be doing a lot of testing and contact tracing. There should be a national initiative for contact tracing, just as there should be a national initiative on securing PPE (personal protective equipment). The responsibility for the abject failure of both of these initiatives rests resolutely on Donald Trump’s doorstep.
Yellow Springs News: So what do you see moving forward?
Dr. Leeds: If you look at Montgomery, Alabama, or rural Oklahoma or Colorado, their latency periods are up. Their bills are arriving. I think we’re not far behind them. I think Ohio will end up in the same boat. We’ll be chasing our tail with lagging indicators. It’s going to be a process of difficult, gradual discovery. If we reopen the pools, or the gyms, or haircutters wear masks and gloves and get back to business…we’ll see how that turns out. It’s an experiment on ourselves: are compromise measures as good as sheltering in place? We’re about to find out. Either way, I think we’ll have a full-fledged second wave. And it may not be the last.
As a physician, I am acutely aware of the effects of economic hardships on my patients, especially the many I care for that live below the poverty line. It’s understandable that some people are disappointed that we “overreacted” by shutting down businesses and sheltering in place and the rest. But are they suggesting that it would have been better to under-react, to spare that disappointment? Again, there’s the math: there are, what, 330 million people in the US? And fewer than 2 million cases documented to date? Think about the second and third wave of the 1918 influenza virus. Most of the fatalities occurred in the third wave. If the lesson we learned from this is not to overreact, then we didn’t learn anything at all.
Yellow Springs News: Thanks for taking the time. It was nice to talk with “the math.”
Dr. Leeds: I’m not the math, I’m just the messenger. And I’m not a mathematician, I’m just a guy that happens to know that two and two equals four.
2 Responses to “COVID-19 in Greene County: Interview with an epidemiologist”
The Yellow Springs News encourages respectful discussion of this article.
You must login to post a comment.
Don't have a login? Register for a free YSNews.com account.















Follow-up questions:
Given the usual pattern of Coronavirus, what months would we expect the second wave to hit in the community – late summer or fall? Would an earlier summer return to school precipitate an earlier second wave. Will this differ in Europe? (We postponed a bike and barge trip in France -Nice to Strasbourg .. and are calculating the relative risk of going in September (We cancelled June, with all the unknowns.)
I’d appreciate a clarification on this sentence.
“Of the 136 who have been tested [as part of the county’s contact tracing], 57% were positive; 42 were negative and 36 were positive.”
Also I’d like to hear what Dr Brannen thinks about the recommendation for people to invest in pulse oximeters and track their readings to watch for pneumonia.
Wow, I find it interesting that we had other outbreak going on and this contact tracing unearthed it.